Table of Contents
- Introduction :
- Renal Circulation :
- Auto Regulation :
- Urine Formation :
- Glomerular Filtration :
- Factors regulating Glomerular filtration rate :
- Tubular Reabsorption :
- Tubular Secretion :
- CONCLUSION :
- References :
- Other Articles :
Introduction :
It is important to eliminate the wastes from the body ,as accumalation of the wastes products in the body causes harmful affect to the body and leads to imbalance and causes diseases . so for the elimination of these wastes from the body it has following ways, wastes may thrown out of the body by sweat mechanism and by formation of urine and faeces .
Urine formation is the main function done by kidneys to purify the blood and expel wastes from body in the form of urine . so , we are going to discuss about the Renal circulation and Urine formation .
Renal Circulation :
In an adult human both the kidneys receive 13,00 ml blood/min which is 26% of the cardiac out put .Blood flow to the kidneys measured by using plasma clearance of para-aminohippuric acid .
Renal blood flow is regulated by auto regulation , nerves innervating the blood vessels has no signifcant role in this mechanism .
NOTE : auto regulation is an intrinsic ability of an organ to regulate it’s own blood . This mechanism is seen in the vital organs like brain ,heart and kidneys .
RENAL BLOOD VESSELS :

Auto Regulation :
As it is the intrinsic ability of an organ to regulate it’s own blood flow , kidneys are more efficient in this mechanism.
In glomerular filtration rate [GFR] the mean arterial blood pressure is maintained between 60 to 180mmHg . It is regulated by two mechanisms they are
- Myogenic response
- Tubuloglomerular feedback
MYOGENIC RESPONSE :
When there is increase in blood flow , it leads to stretching of afferent arteriole which in turn leads to increase in blood flow , it increases calcium ions and leads to influx of these calcium ions from extra cellular into cells . This influx of calcium leads to contraction of smooth muscle of afferent arteriole , which causes contraction of afferent arteriole and leads to decrease in blood flow.

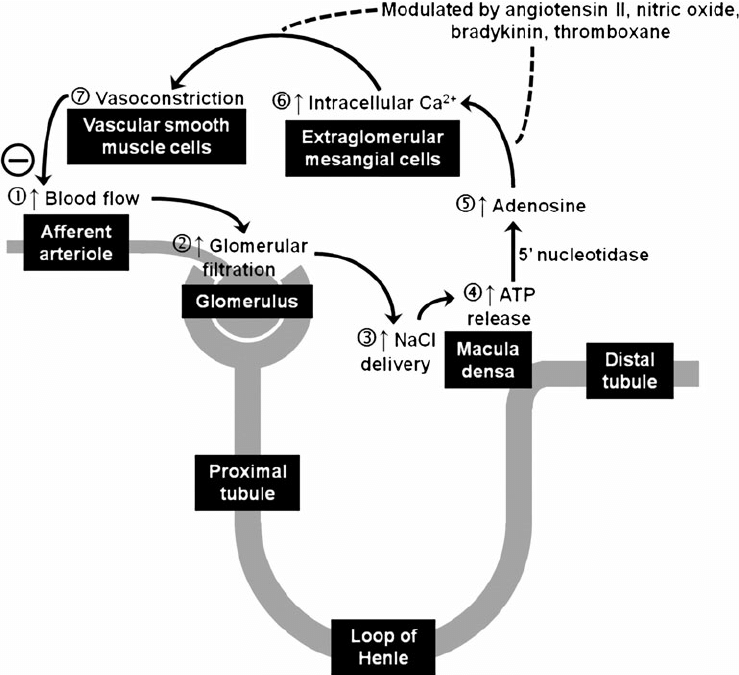
TUBULO GLOMERULAR FEEDBACK :
This feed back is under control of the renal tubule and macula densa . In this macula densa acts as sensor which is sensitive to the sodium and chlorine ions which are detected through the Na+_K+_2Cl- cotransporters.
When there is increase glomerular filtration rate there is increase in the concentration of the sodium and chlorine in the filtrate , this increase leads to release of adenosine from ATP by stimulating macula densa ,which causes contraction of afferent arteriole in presence of adenosine A1 receptors leads to decrease in blood flow and leads to decrease in glomerular filtration rate .
- Factors involved during increase in the GFR :
- Adenosine
- Prostaglandin E2
- Thromboxane
- Hydroxyl icosatetraenoic acid
When there is decrease in the glomerular filtration rate takes place there is decrease in the sodium and chlorine which stimulate macula densa to release PGE2 , Bradykinin and Renin . The PGE2 and bradyakin dilates the Afferent arteriole and the renin acts on angiotensin and leads to constriction of Efferent arteriole . in turn these mechanism leads to increase in GFR and blood flow .
- Factors involved during decrease in the GFR :
- Cyclic AMP [CAMP]
- Nitrous oxide
- Prostaglandin i2
- Atrial natriuretic peptides
NOTE :
- Kidneys blood supply directly arise from the aorta which increases blood flow , nearly 1300 ml blood /min that is 26%of cardiac out put . Kidney are the 2nd organ to receive maximum blood after the liver which receive 30% of the cardiac out put.
- This portal system has double network capillaries those are Glomerular and peritubular capillaries
- Normal capillary pressure is 25 to 30 mm Hg .whereas, renal glomerular capillaries have high pressure that is 60 to 70 mm Hg . This high pressure in the capillaries help in glomerular filtration
- Whereas, peritubular capillaries have low pressure bed 8 to 10 mm Hg which is useful for the reabsorption.
Urine Formation :
It is a blood cleansing function . This is the mechanism of the body through which the blood get purified and eliminate the wastes in the form of urine .In general the normal urine out put is 1 to 1.5 liters /day
- There three stages in urine formation they are :
- Glomerular filtration
- Tubular reabsorption
- Tubular secretion
Glomerular Filtration :
This is also called as the ultra filtration . In this process all substances get filtered except plasma proteins as they have large diameter than the filtration pores in filtration membrane from the glomerulus to Bowman’s capsule . Normally Glomerular Filtration Rate [GFR] is 125 ml/min or 180 L/day .

FILTRATION FRACTION :
Normal filtration fraction is 15 to 20% it is calculated as GFR/Renal plasma x 100
FACTORS FOR FILTRATION :
There are three pressure factors , they are as follows :
- GLOMERULAR CAPILLARIE PRESSURE :This is the pressure exerted by the blood on the glomerular capillaries , which is 60mmHg . It may between 45 to 70 mmHg .
- This glomerular capillary pressure is the highest pressure in the body .
- COLLOIDAL OSMOTIC PRESSURE [ONCOTIC PRESSURE ]: This is the pressure exerted by the plasma proteins on the glomerular capillaries .This is up to 25mmHg .
- HYDROSTATIC PRESSURE IN BOWMAN’S CAPSULE : This pressure is also called as the capsular pressure .This is the pressure exerted by the filtrate enters into bowman’s capsule , this is the pressure which opposes the glomerular filtration rate . This pressure is up to 15mmHg .
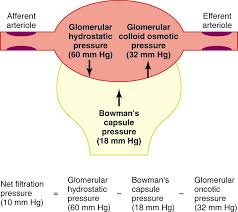
NET FILTRATIO PRESSURE : normal 20mmHg
Net filtration pressure = Glomerular capillary pressure – [colloidal osmotic pressure + Hydrostatic pressure in bowman’s capsule ]
Factors regulating Glomerular filtration rate :
- RENAL BLOOD FLOW :
- controlled by autoregulation through 2 mechanisms they are as follows
- Myogenic response
- tubulo glomerular feedback
- controlled by autoregulation through 2 mechanisms they are as follows
- GLOMERULAR CAPILLARY PRESSURE :
- This is directly proportional to to the GFR and it depends on the renal blood flow and arterial blood pressure
- COLLOIDAL OSMOTIC PRESSURE :
- This is also called as osmotic pressure which is inveresly proportional to the GFR .
- In cases, like Hyper proteinemia and dehydration COP increases
- whereas in hypo proteinemia COP decreases
- HYDROSTSTIC PRESSURE IN BOWMAN’S CAPSULE :
- It is inveresly proportional to the GFR.
- This pressure increase in cases like urethra obstruction edema of kidney beneath renal capsule.
- CONSTRICTION OF THE AFFERENT ARTERIOLE :
- decreased blood flow leads to decreased GFR.
- CONSTRICTION OF THE EFFERENT ARTERIOLE :
- In this case initially GFR increases due to stagnation of blood in the capillaries when all the filtration done further filtration doesn’t occur as efferent arteriole constriction prevent out flow of blood ,no fresh blood enters for further filtration .
- SYSTEMIC ARTERIAL BLOOD PRESSURE :
- Normal range 60 to 180mmHg autoregulatory mechanism fails above or below the mentioned range .
- SYMPATHETIC STIMULATION :
- As both the afferent arteriole and efferent arteriole have sympathetic supply . Stimuation in mild or moderate doesn’t cause any change ,but strong stimulation leads to the release of neurotransmitter nor adrenaline .acts more on the Efferent arteriole than on the afferent arteriole and firstly increases the GFR and then decreases it.
- SURFACE AREA OF THE CAPILLARY MEMBRANE
- it is directly proportional to GFR .
- PERMEABILITY OF CAPILLARY MEMBRANE :
- It is directly proportional to the GFR and in cases like hypoxia permeability increases like even plasma proteins get filtered .
- CONTRACTION OF GLOMERULAR MESENGIAL CELLS :
- These cells are present in between the glomerular capillaries , contraction of these cells leads to decrease in the surface area which in turn leads to the decrease in the GFR.
- HORMONAL AND OTHER FACTORS :
- Factors increasing GFR by vasodilation :
- Atrial natriuretic peptide
- Brain natriuretic hormone
- Dopamine
- Cyclic AMP
- Endothelium derived nitric oxide
- PGE2 [prostaglandin E2
- Factors decreasing the GFR by vasoconstriction :
- Angiotensin II
- Endothelium
- Nor adrenaline
- Platelet – activating factor
- Platelet derived growth factor
- Factors increasing GFR by vasodilation :
Tubular Reabsorption :
This the process through which almost 99% of water and electrolytes get reabsorbed into the blood . This is also called as the selective reabsorption as in this only selected and necessary elements are only get reabsorbed .
- There are two mechanisms for reabsorption :
- Active reabsorption :
- In this ATP get used and it is a uphill gradient .
- Elements like Na+, Ca+, K+, phosphates, sulfates, bicarbonates, glucose, Amino acids, Ascorbic acid , uric acid , ketone bodies .
- Passive reabsorption :
- No use of ATP , downhill gradient
- Elements like chloride , urea , water
- Active reabsorption :
ROUTES OF REABSORPTION :
There are two routes through which the substances get reabsorbed from the tubular lumen to the peritubular capillary .
- Transcellular route
- paracellular route
TRANSCELLULAR ROUTE :
In this the substances from the tubular lumen get transported into the tubular cell through the apical surface of the cell membrane and from there to capillary through the interstitial fluid.
PARACELLULAR ROUTE :
Reabsorption of the substances from the tubular lumen to the interstitial fluid through the lateral intercellular spaces by tight junctions and then into the capillary .

REGULATION OF TUBULAR REABSORPTION :
- Regulated by 3 factors
- Glomerulotubular balance
- Hormonal factors
- Nervous factors
Glomerulotubular balance :
Balance due to the osmotic pressure in peritubular capillaries leads to to the increase in the GFR which in turn increase plasma protein in glomerulus which increases the osmotic pressure causes the increase in the reabsorption
Hormonal Factor :
- Aldosterone : Increase Na+ reabsorption in the ascending limb of loop of Henle, DCT and collecting duct
- Angiotensin II : Increase Na+ reabsorption in the PCT , DCT, collecting duct and thick ascending limb of loop of Henle
- Antidiuretic hormone : Increases the H2O reabsorption in the DCT and collecting duct.
- Atrial natriuretic factor and brain natriuretic factor : Decreases Na+ reabsorption .
- Parathormone : Increase Ca+, Mg+, H+ reabsorption and decrease in phosphate reabsorption.
- Calcitonin : Decrease in Ca+ reabsorption.
Nervous Factor :
Sympathetic system which indirectly stimulates the JG cells and release renin which acts on the angiotensin II which in turn leads to increase in reabsorption .
SITE OF REABSORPTION :
- PCT : Glucose , amino acids, Na+, K+, Ca+, bicarbonates, chlorides, phosphates, urea, uric acid, H2O.
- Loop of Henle : Na+ and Cl-
- DCT : Na+, Ca+, bicarbonates, H2O.
- Collecting duct : Na+, urea and water
Tubular Secretion :
Tubular secretion is a vital renal process in which the kidneys actively transport substances from the blood into the tubular fluid within the nephrons, facilitating the excretion of waste products and regulation of blood composition. This mechanism complements filtration and reabsorption, ensuring efficient waste removal and maintenance of homeostasis. This process is also called as tubular excretion.
Primary Sites of Tubular Secretion:
- Proximal Convoluted Tubule (PCT): Secretes hydrogen ions (H⁺), ammonium ions (NH₄⁺), creatinine, urea, and certain drugs.
- loop of Henle : Secretes urea.
- Distal Convoluted Tubule (DCT) and Collecting Ducts: Secrete potassium ions (K⁺) and hydrogen ions (H⁺), aiding in electrolyte and acid-base balance.
Mechanisms of Tubular Secretion:
- Active Transport: Utilizes ATP-driven pumps and transporters to move substances against their concentration gradients from peritubular capillaries into the tubular lumen.
- Passive Diffusion: Allows lipid-soluble substances to diffuse passively across cell membranes into the tubular fluid.
Functions of Tubular Secretion:
- Waste Removal: Eliminates substances not effectively filtered by the glomerulus, such as certain drugs and toxins.
- Electrolyte Balance: Regulates blood levels of potassium and hydrogen ions, crucial for nerve function and muscle contraction.
- Acid-Base Regulation: Secretes hydrogen ions and reabsorbs bicarbonate ions to maintain the body’s pH within a narrow, optimal range.
CONCLUSION :
Renal circulation and urine formation are fundamental processes that the kidneys utilize to maintain the body’s internal balance, remove waste, and regulate various physiological parameters.
Renal Circulation:
Blood enters the kidneys through the renal arteries, which branch off from the abdominal aorta. These arteries divide into smaller arterioles, leading to the glomeruli networks of capillaries within the nephrons, the functional units of the kidneys. The glomeruli filter the blood, initiating urine formation. After filtration, blood exits the glomeruli via the efferent arterioles, which further branch into peritubular capillaries surrounding the renal tubules. This arrangement facilitates the exchange of substances between the blood and the tubular fluid, crucial for reabsorption and secretion processes.
Urine Formation:
Urine formation occurs through three sequential processes:
- Glomerular Filtration: Blood pressure forces water and small solutes from the glomeruli into Bowman’s capsule, forming the filtrate. This process excludes larger molecules like proteins and cells.
- Tubular Reabsorption: As the filtrate passes through the renal tubules, essential substances such as glucose, amino acids, and ions are reabsorbed into the peritubular capillaries. This selective process ensures the retention of vital nutrients and maintains fluid and electrolyte balance.
- Tubular Secretion: Additional waste products and excess ions are actively transported from the peritubular capillaries into the tubular fluid. This step enhances the elimination of certain substances, including drugs and metabolic waste products.
The processed filtrate, now urine, collects in the renal pelvis and is transported to the bladder via the ureters. The bladder stores urine until it is expelled from the body during urination.
In summary, renal circulation delivers blood to the kidneys for filtration, while the processes of filtration, reabsorption, and secretion within the nephrons meticulously regulate the composition of the body’s fluids, remove waste, and maintain homeostasis.
References :
- Physiology, Renal Blood Flow and Filtration – NCBI
- Renal Blood Flow and Oxygenation – PMC
- Kidney Circulation Overview – ScienceDirect
- Regulation of the Renal Circulation – Kidney International
- Renal Blood Flow During Exercise – Journal of Applied Physiology
Other Articles :
Over view : Internal Structure of Kidney
Gait Abnormalities: Over View On Types of Gait Abnormalities
Kidney : Anatomy and Clinical Significance
100+ AYURVEDIC DRUGS ACCORDING TO BAMS NCISM SYLLABUS
Pharmacological Insights into Charakokta Dashemani: Part -1 (01 – 20 Dashemani Mahakashaya)
Pharmacological Insights into Charakokta Dashemani: Part -2 (11- 20 Dashemani Mahakashaya)
Pharmacological Insights into Charakokta Dashemani: Part -3 (21 – 30 Dashemani Mahakashaya)
Pharmacological Insights into Charakokta Dashemani: Part -4 (31- 40 Dashemani Mahakashaya)
Pharmacological Insights into Charakokta Dashemani: Part -5 (41- 50 Dashemani Mahakashaya)






Keep up the great work, I read few blog posts on this site and I think that your blog is really interesting and holds sets of good information.
Thank you so much @drover for your great appreciation